They report that sources of their stress include finding appointments for patients as well as feeling caught between doctors and patients demands.Ī 2013 survey of 508 employees working for 243 health care employers found that 60 percent reported job burnout and 34 percent planned to look for a different job. Most receptionists feel that physicians do not appreciate the complexity of their work. On the front lines of practice, receptionists also have stressful jobs, with 68 percent reporting verbal abuse from patients. Studies show that 34 percent of hospital nurses and 37 percent of nursing home nurses report burnout, compared with 22 percent of nurses working in other settings. The 2013 RAND Corporation survey showed 30 physician practices found that electronic health record (EHR) technology has worsened professional satisfaction through time-consuming data entry and interference with patient care.Ī more recent professional life survey of ACC members found EHR challenges continue to keep clinicians up at night, along with work-life balance, maintenance of certification, reimbursement challenges, prior authorization and quality reporting.īurnout affects not only physicians but also other members of the health care workforce. Physicians spend more time on non-face-to-face activities (in-box management of labs and documents, messages and medication refills) than with patients. In a survey conducted in the Annals of Family Medicine, 43 percent of physicians reported spending over 30 percent of their day on administrative tasks. In a national survey conducted by Physician Wellness Services and Cejka Search, 87 percent of physicians named the leading cause of work-related stress and burnout as paperwork and administration, with 63 percent indicating that stress is increasing. According to a 2013 RAND Corporation survey, the principal driver of physician satisfaction is the ability to provide quality care. 
Professional burnout is characterized by loss of enthusiasm for work, feelings of cynicism and a low sense of personal accomplishment, and is associated with early retirement, alcohol use and suicidal ideation. 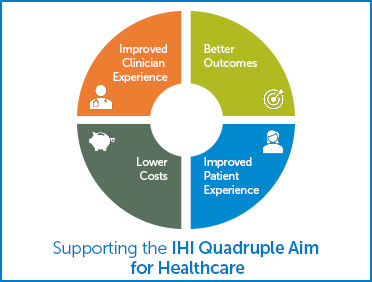
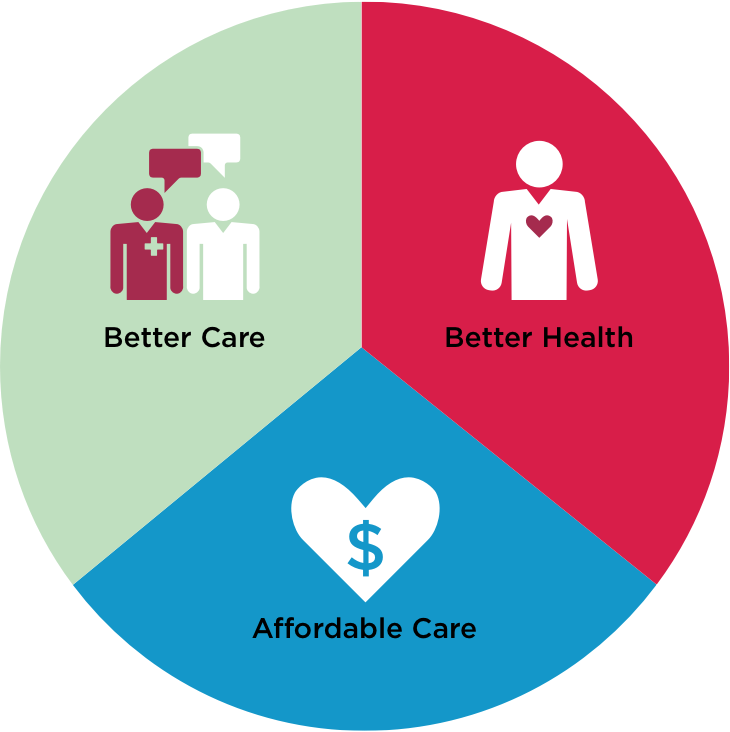
Caregiver burnout among nurses and other team members may contribute to the overuse of resources and increased costs of care. The backbone of any effective health care system is an engaged and productive workforce, and members of the health care workforce have reported widespread burnout and dissatisfaction.īurnout among the health care workforce can threaten the success of Triple Aim by lowering patient satisfaction and increasing the possibility of errors. Although each of the components is necessary to succeed in the new era of health care, a key component is missing – the care providers. Working on the three elements of the Triple Aim has not been without its challenges. Reducing the per capita cost of health careĪs health systems were grappling with the challenge of improving population health while simultaneously lowering health care costs, the Triple Aim was adopted as a set of principles for health system reform.Improving the patient experience of care (including quality and satisfaction).It centered around three overarching goals: Berwick, MD, MPP, FRCP, and colleagues provided this Triple Aim as a framework for the delivery of high-value care. During this transition, there has been focus on the Triple Aim, an approach to optimize health system performance. Changes in regulations, patient access to information and technological advances have led to an increased focus on patient experience. Over the last decade, health care has seen a shift in the way providing care is addressed. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
